Residents practice surgical skills in virtual reality
|
“When the patient complains of discomfort, you can give more sedation,” John Migaly, M.D., advised the first-year residents, “But if you perforate the colon, it’s ‘game over.’” Migaly, assistant professor of surgery, was not being callous. He was instructing the new MDs on the intricacies of colonoscopy using a video simulator that feels, sounds and looks like a real person and procedure.
|
 Photo by Kelly & Massa
John Migaly, M.D., trains first-year surgical resident Jay Simhan (right) to perform a colonoscopy using a new video simulator.
|
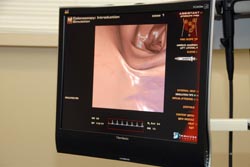 Photo by Kelly & Massa
A video monitor shows the user where the scope is in the simulated large intestine.
|
Just as in a real procedure, the students watch a video monitor as the scope travels through the body to its destination. The simulator can be programmed to portray cases according to gender, age and disease or medical condition. Built-in force and resistance make it feel as if it’s a real patient and various sounds, like coughing and moaning, convey discomfort or pain. The residents can ask the simulator for tips and practice at varying skill levels. |
|
Another advantage of the simulators is objective, computer-based evaluation. Surgical skills are often difficult for professors to assess. The simulators chart and analyze each student users’ performance and progress in detail and over time. Students and teachers can figure out exactly where improvement is needed and adjust training accordingly. The simulators are now part of the curriculum for first-year surgical residents, explained Richard Milner, director of the surgical skills lab, to address the need for more clinical training in colonoscopy and other minimally invasive procedures, which are fast becoming some of the most commonly performed medical procedures. Numerous surgical procedures are now minimally invasive, thanks to laparoscopes and endoscopes, sparing patients from major surgery and the accompanying lengthy hospital stays and recoveries.
|
|