Training eases end-of-life conversations with families
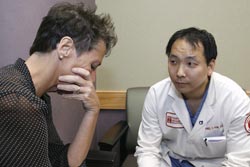 Photo by Ryan Brandenberg/Temple University
Temple resident Daniel Kim, M.D., (right) talks with an actor patient during a simulation about organ donation.
|
One of the most important, yet most difficult conversations for a doctor comes when approaching a family about organ donation when a patient is diagnosed as brain-dead. Yet sensitive, thoughtful communications between doctors and the families of these patients could potentially improve organ donation rates. Prior research has correlated a family’s understanding of brain death and donation consent rates.
|
|
So far, Goldberg and her colleagues have found that just two extra hours of communications training in end-of-life issues is valuable. Residents were tested at Temple’s Institute for Clinical Simulation and Patient Safety.
One group of residents participated in a simulated conversation explaining the brain death of a loved one to families, while another group received no specialized training. Eight weeks later, both groups participated in formal videotaped family communication simulations regarding brain death. Their performances were reviewed and rated by professionals considered to be experts in this area. Residents who had received previous training scored 20 percent better than those residents who had not received any training.
|
|