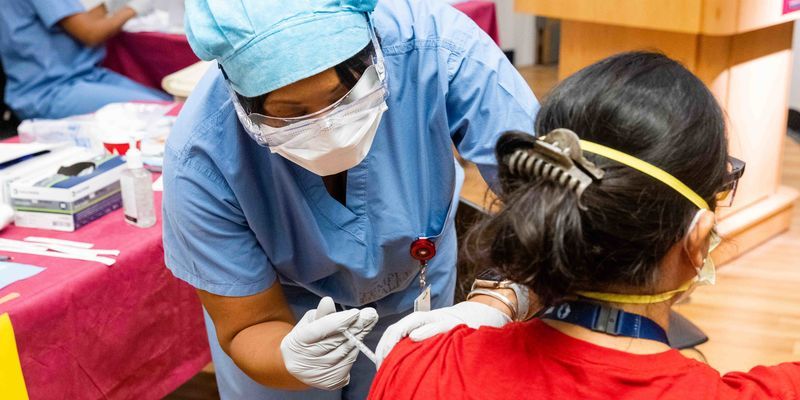
The COVID-19 vaccines: explained
Temple experts share the top 7 things you need to know about the COVID-19 vaccines.
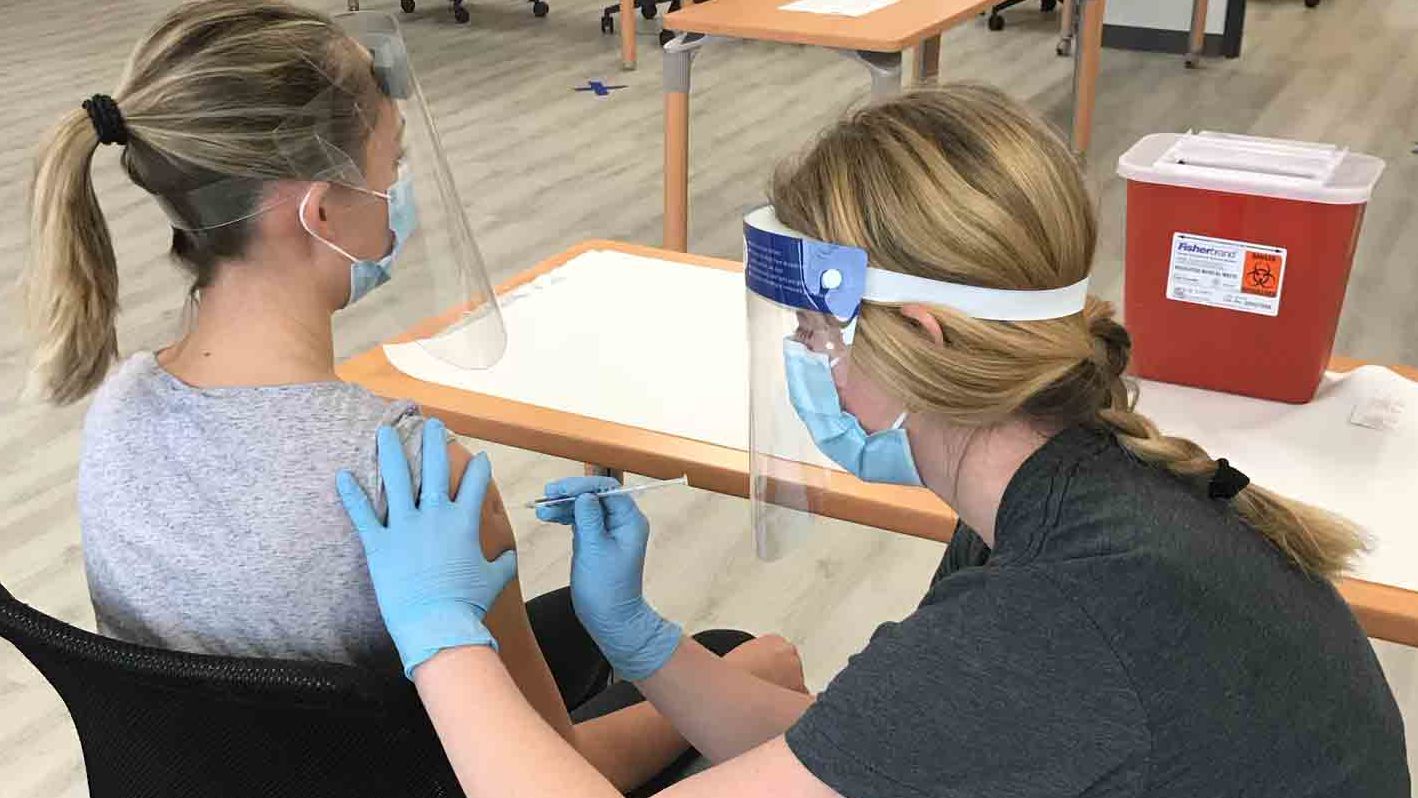
Three Temple experts have information to help you sort through the info about the COVID-19 vaccine rollout. Krys Johnson, assistant professor of instruction in the Department of Epidemiology and Biostatistics in the College of Public Health, focuses on mitigating health disparities through community-based research. Jason Gallagher, a clinical professor in the School of Pharmacy, treats patients as a pharmacy specialist focused on infectious diseases at Temple Health. Sarah Bass, associate professor of social and behavioral sciences and director of the Risk Communication Laboratory in the College of Public Health, uses commercial marketing methods to develop messaging around public health issues.
Here is what they had to say.
- There are three vaccines that have been shown to be the most effective in clinical trials.
Two—mRNA vaccines from Pfizer and Moderna—were fast-tracked for FDA approval in the U.S., and both have now received FDA approval. “A third one—the AstraZeneca Oxford vaccine—is right behind both of them and is a weakened adenovirus vaccine,” Johnson said. “But that has not been submitted for FDA approval yet in the U.S.”
- The Pfizer and Moderna vaccines are different from the vaccines you’ve had before.
You have likely received vaccines, such as those for influenza, that contain small amounts of inactivated virus, which are designed to trigger your body into creating an immune response.
The COVID-19 mRNA vaccines work differently. They contain no virus at all, but instead contain RNA that targets the specific spike-shaped protein that gives coronavirus its name.
“The mRNA tells your body how to recognize COVID-19 if you come into contact with it,” said Johnson. “It gives your body the recipe of how to create the antibodies and how to prepare itself.”
- You need two doses for the vaccine to be effective.
“mRNA is a very finicky and fragile particle, so it does its job and then it’s gone,” said Johnson.
“Studies so far have shown some protection from the first dose,” said Gallagher. “But we don’t know how long that will last. All of the studies so far have used two doses.”
- These vaccines are not new.
Some have expressed concern that the COVID-19 vaccines were developed and tested over the past 11 months, meaning they have not been sufficiently screened. Johnson explained that’s not the case: “This vaccine was created over 17 years. It just so happened that we were at the point where we could use the technology that we built up over the past two decades as part of our efforts to create a universal flu vaccine to develop a COVID vaccine.”
- The COVID-19 vaccines are extremely effective.
“Out of 20,000 folks who received the vaccine in the Pfizer trials, there was only one single severe case of COVID-19,” Johnson said. “That is better than our flu vaccine, which can typically prevent between about 30% and 70% of cases.”
“In a trial with 15,000 vaccinated people, the Moderna vaccine had no cases of severe infection, versus 30 in the placebo group,” Gallagher added.
“For us to come out of the gate with two different vaccines that can prevent up to 90% or 95% of cases is astonishing,” Johnson added.
- You may have side effects … but this usually just means the vaccine is working.
“When you have a cold or the flu, the reason you feel sick is due to the release of cytokines, which are substances produced by our cells to communicate with each other. Because your immune system is working so hard to fend off an infection, it feels like our bodies are going into overdrive—this is what causes the fever, the fatigue, the aches,” said Gallagher.
With the COVID-19 vaccine specifically, “there are significant percentages of people reporting mild to moderate fatigue, malaise and fever the day after they’re vaccinated. But a little bit of pain reliever will help that,” he added.
- Distribution and accessibility to the vaccine could be challenging, but the greatest challenge may be educating people about the vaccine’s benefits.
“Vaccines have been the subject of controversy over the past 15 to 20 years, so some people distrust them,” said Bass. “You have to listen to people and try to frame messages around what’s important to them: being around their families, taking care of their elderly parents, getting back to normal life.”
“It’s trite to say there’s no cure for the common cold,” said Gallagher. “But the truth is that the way out of viral diseases is vaccination. This may be a disease that we deal with for the rest of our lives, but it shouldn’t be anything like it is right now, because helping to stop transmission is an enormous advantage.”
Gallagher, Bass and Johnson all agree: “There really is a light at the end of the tunnel,” Gallagher said. “If we hunker down for the next few months, we can enjoy the next year.”
—Sonia Belasco